Myelography – Procedure, Uses, Indications, Spinal Stenosis Diagnosis & Ayurvedic View
Abstract
Spinal stenosis is a silent narrowing of the vertebral canal, where the body’s central river of nerves is gradually compressed by time, degeneration, or structural change. As space diminishes, symptoms emerge—radiating pain, numbness, weakness, and neurogenic claudication—signaling distress within the spinal corridor. While MRI often leads modern imaging, myelography remains a powerful diagnostic ally. By introducing contrast into the subarachnoid space, myelography outlines the spinal cord and nerve roots with striking clarity, especially in complex or postoperative cases. It transforms hidden compression into visible architecture, guiding precise clinical decisions and offering a dynamic map for surgical or interventional planning. Let’s discuss this in detail!
Introduction
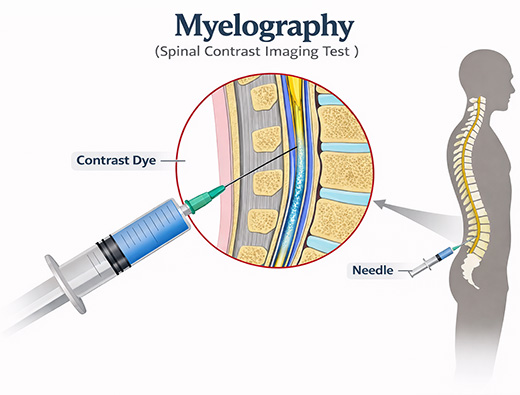
Myelography is a specialized diagnostic imaging technique used to evaluate disorders of the spinal canal, nerve roots, and spinal cord, particularly in conditions such as spinal stenosis, herniated discs, and tumors. The procedure involves injecting contrast dye into the subarachnoid space followed by X-ray or CT imaging to enhance visualization of neural structures. Although Magnetic Resonance Imaging has largely replaced it as a first-line tool, myelography remains significant in postoperative patients or those with MRI contraindications. Lumbar spinal stenosis affects nearly 11% of adults over 60, making precise imaging essential. Myelography provides dynamic, detailed assessment, guiding accurate diagnosis and surgical planning.
What Happens During The Procedure?
The procedure typically takes between 30 to 60 minutes, followed by a period of observation. It is performed by a radiologist using fluoroscopy (a real-time X-ray movie) to ensure the needle is placed with mathematical precision. Here is the step-by-step breakdown of what happens:
- Positioning and Numbing– You will be asked to lie on your stomach (prone) or on your side in a fetal position. The radiologist cleans your lower back with an antiseptic and applies a local anesthetic. You’ll feel a quick sting and burn from the numbing medicine, similar to a dental freezing. After this, you should only feel pressure, not sharp pain.
- The Spinal Tap (Needle Placement)– Using the fluoroscope for guidance, the doctor inserts a thin, hollow needle into the subarachnoid space (the area surrounding the spinal cord filled with fluid). Sometimes, a small amount of cerebrospinal fluid (CSF) is removed for laboratory testing before the dye is added.
- Injecting the Contrast Dye– The radiologist injects a water-soluble "contrast" dye through the needle. Some patients report a brief "warm" or "flushing" sensation as the dye enters the spinal canal.
- Capturing the Images– This is the "active" part of the procedure. The needle is removed, and the X-ray table may be tilted. By tilting the table, gravity moves the dye up and down your spine to coat different nerve roots. You may be asked to roll slightly or hold your breath while X-rays are taken from various angles.
- The Post-Myelogram CT (Optional but Common)– In most modern hospitals, you are moved immediately to a CT scanner while the dye is still "fresh" in your system. This creates a 3D map that is much more detailed than the flat X-ray images.
Post-Procedure Recovery
Once the imaging is done, you aren’t quite finished yet. There is a specific recovery protocol:
- Observation: You will stay in a recovery room for 1 to 2 hours.
- The "Head Up" Rule: You must keep your head elevated (usually at a 30° to 45° angle). This prevents the dye from traveling too high into the brain area, which helps prevent headaches.
- Hydration: You’ll be encouraged to drink lots of water to help your kidneys filter out the contrast dye.
Potential Side Effects
While generally safe, the most common "hiccup" is a post-lumbar puncture headache. This happens if a little bit of spinal fluid leaks from the needle site. It usually goes away with rest and caffeine, but it’s why the "head up" rule is so strictly enforced!
Indications
Here are the primary indications for a myelography procedure
- MRI Contraindications: Used for patients with incompatible medical implants (pacemakers, certain aneurysm clips, cochlear implants) or severe claustrophobia.
- Evaluation of Spinal Stenosis: Specifically used to visualize the narrowing of the spinal canal and the resulting pressure on the spinal cord or nerve roots.
- Post-Surgical Assessment: Best for patients with existing metal hardware (rods, screws, or plates) that creates "magnetic artifacts" or blurriness on an MRI.
- Dynamic/Positional Imaging: Allows for imaging while the patient is flexed, extended, or tilted to see how movement affects nerve compression.
- Detection of CSF Leaks: Used to pinpoint the exact location of a cerebrospinal fluid leak in patients suffering from chronic "positional" headaches.
- Nerve Root Avulsions: Identifying if nerve roots have been torn away from the spinal cord following severe trauma or accidents.
- Tumors and Cysts: Visualizing the "silhouette" of the spinal cord to identify masses, such as arachnoid cysts or spinal cord tumors, that are compressing neural tissue.
- Disc Herniation Confirmation: Used when MRI results are inconclusive or do not fully explain a patient’s clinical symptoms (e.g., unexplained leg weakness or numbness).
- Surgical Mapping: Providing a highly detailed "road map" for surgeons to determine the exact level of the spine that requires decompression.
Myelography Interpretation
|
Finding |
Visual Appearance |
Clinical Meaning |
|
Extradural Defect |
A "dent" or indentation from the outside into the dye column. |
Pressure from herniated discs, bone spurs, or thickened ligaments. |
|
Intradural-Extramedullary |
Dye is pushed aside; it creates a "crescent" or "meniscus" shape. |
A growth inside the sac but outside the cord (e.g., a meningioma). |
|
Intramedullary |
The spinal cord appears widened; dye lanes are squeezed thin. |
Swelling or a mass inside the spinal cord itself (e.g., a tumor or cyst). |
|
Nerve Root "Cut-off" |
The small "sleeves" of dye for specific nerves are missing. |
A nerve is pinched or blocked at its exit point from the spine. |
|
Hourglass / Block |
Dye narrows to a thin thread or stops moving entirely. |
Severe spinal stenosis; the canal is nearly choked off. |
|
Extravasation |
Dye "spills" or leaks outside the spinal canal boundaries. |
A tear or hole in the protective membrane (CSF leak). |
Ayurveda’s View
In Ayurveda, spinal stenosis and the symptoms visualized in a myelogram are primarily viewed as a manifestation of Vata Vyadhi (disorders caused by an imbalance of the Vata dosha, which governs movement and the nervous system). While Ayurveda doesn’t have a "needle-and-dye" diagnostic like myelography, it interprets the structural narrowing and nerve pain through the lens of Dhatu Kshaya (tissue depletion) and Margavarana (blockage of channels). Ayurvedic herbs that help in managing vata vyadhi and strengthen the spinal cord and nerves are as follows :-
1. Guggulu (Commiphora mukul)
This is Known for its Lekhana (scraping) property. It "scrapes" away Ama (toxins) and excess Kapha from the Srotas (channels), physically clearing the "blockage" in the spinal canal. It contains guggulsterones, which act as potent anti-inflammatories. Research suggests they inhibit NF-kappaB, a protein complex that triggers the inflammatory response, thereby reducing swelling around pinched nerves.
2. Ashwagandha (Withania somnifera)
A premier Balya (strength-giving) and Rasayana (rejuvenating) herb. It pacifies Vata and nourishes the Majja Dhatu (bone marrow and nervous system) to prevent further degeneration. It is Classified as an adaptogen. It contains withanolides which have neuroprotective effects. It promotes dendritic arborization (growth of nerve cell branches), helping the body repair the "frayed" nerves caused by chronic compression.
3. Shallaki (Boswellia serrata)
This herb is Primarily used for Shothahara (reducing edema) and Sandhi-Vata (joint-related Vata issues). It improves blood circulation to the joints. Also it contains boswellic acids, which are specific inhibitors of 5-LOX (5-lipoxygenase). Unlike modern NSAIDs, they reduce inflammation without irritating the stomach lining, making them ideal for long-term spinal pain management.
4. Nirgundi (Vitex negundo)
Nirgundi is highly regarded for its Vata-hara and Vedana-sthapana (analgesic) properties. It is considered "hot" in potency, which helps "melt" the cold, stiff nature of spinal stenosis. This is rich in flavonoids and alkaloids that act on the central nervous system to dampen pain signals. It has been shown to reduce oxidative stress in the spinal tissues, slowing down the "wear and tear" of the vertebrae.
5. Rasna (Pluchea lanceolata)
Specifically mentioned in ancient texts as the best herb for Amavata and Vata disorders of the lower limbs. It helps move stagnant energy from the hips down to the feet. It contains quercetin and isorhamnetin. These compounds help stabilize cell membranes and prevent the release of chemicals that cause nerve irritation and the "shooting pain" associated with sciatica.
6. Bala (Sida cordifolia)
It focuses on the "Bala" (strength) of the Snayu (ligaments and tendons). By strengthening the structures holding the spine together, it prevents the "slipping" or collapsing that narrows the canal. This contains small amounts of ephedrine alkaloids and phytosterols. These act as mild muscle relaxants and stimulants that improve the tone of the deep spinal muscles, providing better structural support for the bony canal.
7. Dashmoola (The Ten Roots)
It is the ultimate Vata-hara (Vata-destroyer). It is specifically used for Shvasa-Kasa and Kati Graha (stiffness in the lower back). It works on the principle of synergy—five “Great Roots” (Brihat Panchamoola) treat the upper body and nerves, while five “Small Roots” (Laghu Panchamoola) treat the lower body and inflammation. Dashmoola acts as a broad-spectrum anti-inflammatory and analgesic. It modulates the body’s immune response and inhibits the production of prostaglandins (chemicals that cause pain). Because it contains various phytochemicals like sitosterols and flavonoids, it helps in reducing “perineural edema”—the swelling of the tissue around the nerves that the myelogram identifies.
Conclusion
At last it can be concluded that despite the prevalence of MRI, myelography remains a cornerstone in spinal diagnostics, particularly for complex cases of spinal stenosis. By providing a high-contrast silhouette of the subarachnoid space, it excels where other methods fail—specifically in patients with metal implants or those requiring dynamic, weight-bearing assessments. While invasive, its ability to pinpoint nerve impingement and CSF leaks ensures precise surgical planning. Whether viewed through the lens of modern radiology or as a means to identify Margavarana (blockage) in Ayurveda, myelography provides the definitive anatomical "map" necessary for restoring mobility and improving the patient’s quality of life.



